Your patient is a 76 year old female who is experiencing shortness of breath.
1. List 3 serious conditions which could be responsible for her shortness of breath.
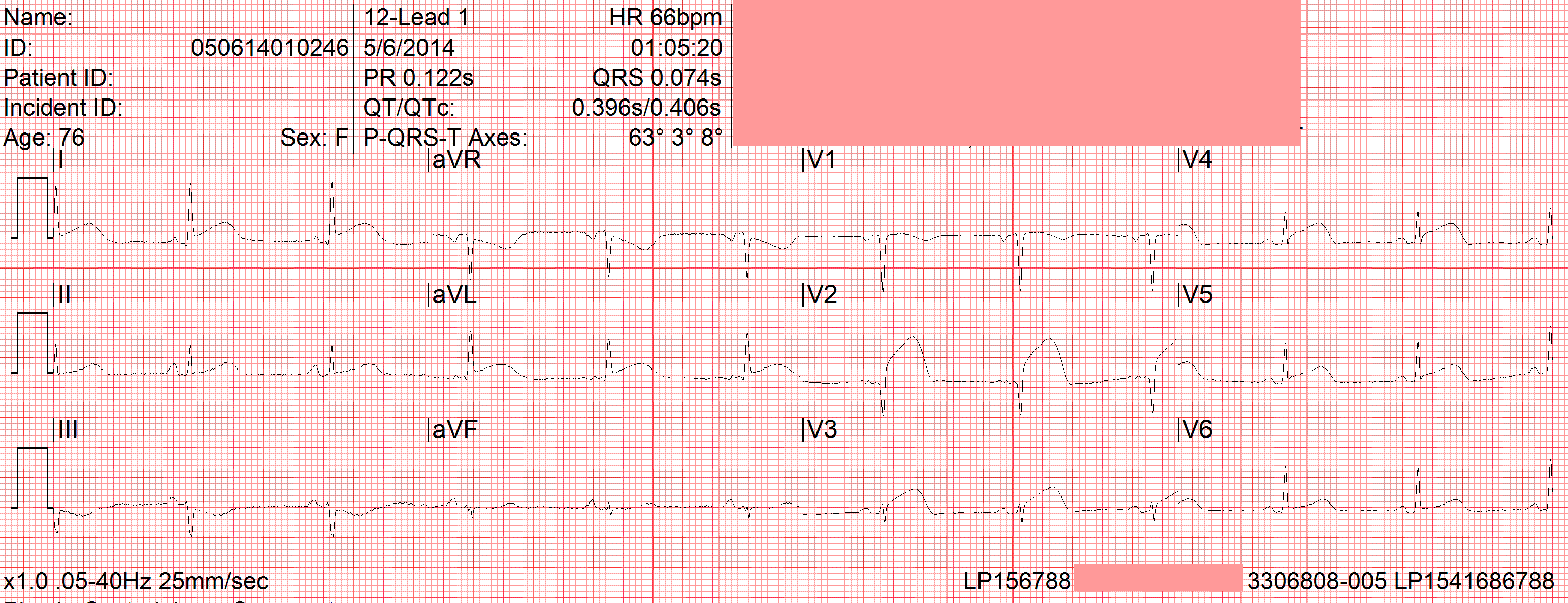
Answer 1. Pulmonary embolism You record the following ECG. (Right click on the image, then select “Open in new window” to enlarge) What is your interpretation of the ECG? Rhythm – normal sinus rhythm What are your treatment priorities? 1. Notify receiving facility What should you anticipate with this patient presentation? Patients who present with anterior wall STEMI are at high risk for developing ventricular dysrhythmias, sudden cardiac arrest, and pulmonary edema. Be prepared to aggressively treat with electrical therapy and CPAP, respectively. Be sure to notify the receiving facility early and continuously monitor the patient’s mental and respiratory status, cardiac rhythm, and vital signs. Feel free to post any questions or comments you may have.
2. Acute myocardial infarction
3. Pulmonary edema
4. Sepsis
5. Pneumonia
6. COPD / asthma
Answer
Axis – normal axis
Chamber size – none
Conduction problems – none
Ischemia – anterolateral STEMI; reciprocal ST depression III, aVF
Miscellaneous – none
Answer
2. Transmit ECG
3. Begin transport to cardiac intervention center
4. Administer NTG and ASA
5. Place combo pads
6. Gain IV access
7. Notify / consult
8. Obtain additional traces
Answer